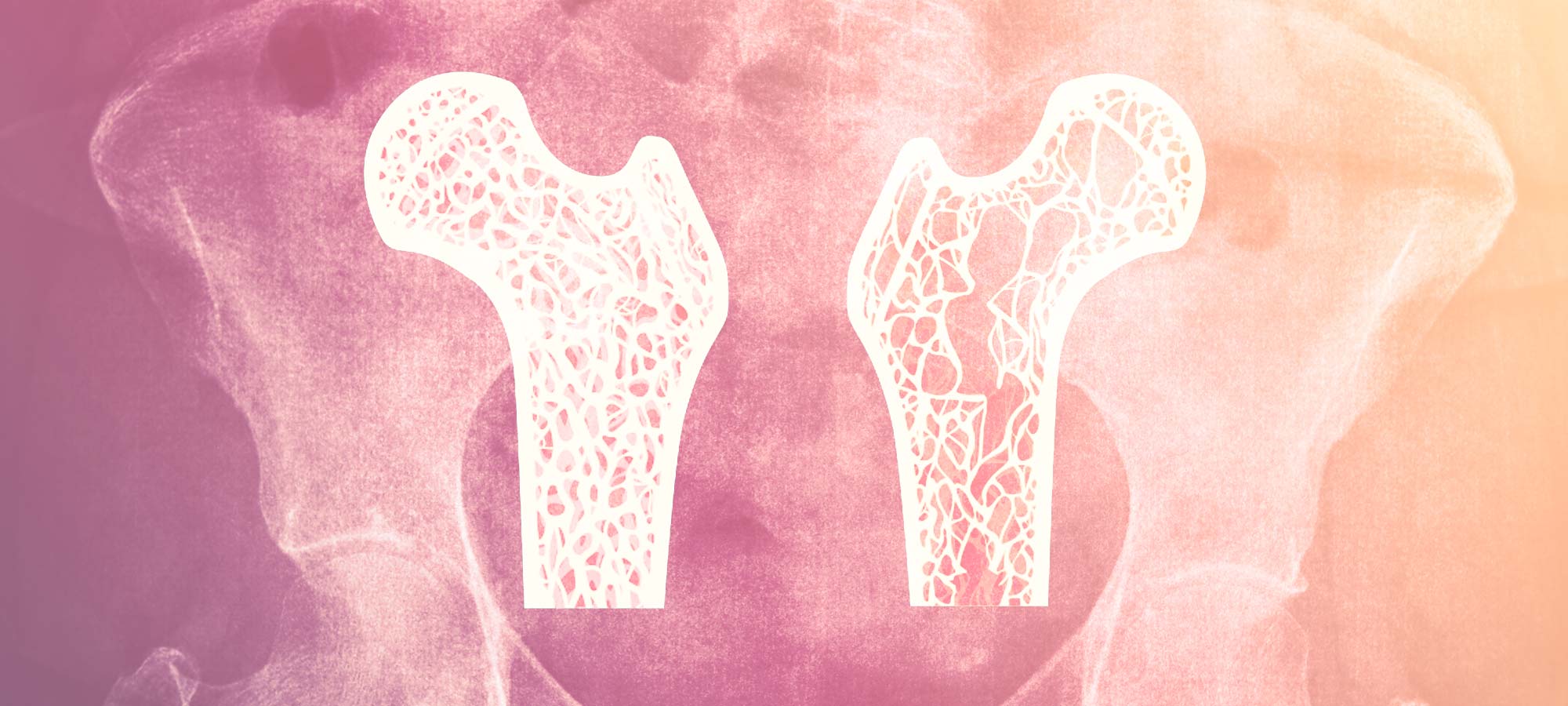
Unfortunately, it’s not something that is commonly tested for unless there are certain risk factors or clinical signs present that suggest investigations are warranted. Part of the challenge with this is that it is not as simple as getting a blood test – it requires a body scan using special equipment (called a DXA, which stands for dual-energy x-ray absorptiometry).
The sooner we identify poor bone health, the better – for several reasons. Firstly, you don’t want to wait until loss of bone mineral density has progressed all the way to osteoporosis and you’ve had a fracture. This can greatly impact quality of life. Secondly, changes made earlier in life to optimise your bone health can have a greater impact than they do later on. For example, making sure our bones are as healthy as possible by around 30 years of age can help to prevent or delay the development of osteopenia later in life.
So, you actually don’t want to wait for there to be a problem. The best time to support your bone health is now – regardless of your age.
Factors that increase your risk
Unfortunately, females are at a higher risk of developing osteopenia – particularly when estrogen is low. This is one reason why we typically hear about osteoporosis rates increasing post menopause. However, certain hormonal conditions or disruptions that involve lower estrogen levels in pre-menopausal women are also a problem – a symptom of this can include a lack of periods or infrequent periods. This can occur with chronic undereating and/or overexercising (either intentional or unintentional), for example.
There are many other factors that can contribute to low bone mineral density too, including:
- Nutritional factors – particularly inadequate calcium, magnesium and boron intake and vitamin D deficiency
- Low muscle mass
- A lack of regular weight-bearing movement
- Smoking
- Long-term use of certain medications, such as steroids and proton-pump inhibitors (a common type of medication that lowers stomach acid)
- Certain medical conditions that are undiagnosed/untreated, such as coeliac disease.
Importantly, many of these factors are within our control – including how we eat and how we move.
How to support strong bones throughout your life
The nutrients essential to our bone health include calcium, magnesium, boron, vitamin D and vitamin K2. Foods abundant in calcium encompass a variety of options including leafy greens like broccoli and kale, as well as almonds, seeds like chia and sesame, tahini, sardines and salmon with edible bones, and firm tofu prepared with calcium salt.
If your digestive system permits, dairy products such as kefir, hard cheese, and yogurt also serve as calcium sources. For those prioritising bone health, fermented dairy alternatives like kefir and unsweetened yogurt are preferred, as they not only offer calcium but also contain some vitamin K2. Vitamin K2 is naturally produced by bacteria in our gut, however, as this is variable, food sources such as fermented foods, eggs, chicken and beef are important to include. Magnesium is found in leafy green vegetables, nuts and seeds (and butters/spreads made from these), seaweeds (such as kelp) and cacao.
Equally as important, if not more important to bone health is muscle mass. Most often it’s a case of the bigger our muscles, the stronger our bones. Regular weight bearing exercise improves and maintains bone density. Resistance training activities such as weights, yoga, Pilates, skipping, dancing, walking and sports like tennis, basketball and netball will help to activate our osteoblasts – the cells that form new bones – and support good tensile strength.
Please note:
If you suspect you may have a condition that could be impacting your bone health, please consult with your GP. It’s important not to make any changes to prescribed medications without consulting your medical practitioner.